Endometriosis is a chronic, often painful condition in which tissue similar to the lining of the uterus grows outside the uterus – on the ovaries, fallopian tubes, or other pelvic organs. Millions of women worldwide live with this condition for years without a correct diagnosis. Knowing how to check for endometriosis symptoms early is one of the most important steps toward getting the right treatment and improving quality of life.
Because the symptoms of endometriosis closely mimic other conditions like ovarian cysts, irritable bowel syndrome, or even general lower back pain, it is frequently misdiagnosed or dismissed. This guide walks you through every major symptom, how to recognise it, what causes it, and when to seek professional help.
Not sure these symptoms match yours?
Try our FREE symptoms checker to compare what your pain might
What Is Endometriosis and Why Does It Happen?
Endometriosis occurs when endometrial like tissue implants itself outside the uterus and responds to hormonal changes during the menstrual cycle, thickening, breaking down, and bleeding but with no way to exit the body. This trapped blood causes inflammation, scar tissue (adhesions), and, in some cases, cysts known as endometriomas or “chocolate cysts”.
The exact cause remains unclear, but theories include retrograde menstruation (backward flow of menstrual blood), immune system dysfunction, genetic predisposition, and hormonal imbalances such as oestrogen dominance. Women with a close relative who has endometriosis are at a significantly higher risk.
How to Check Endometriosis Symptoms Key Warning Signs
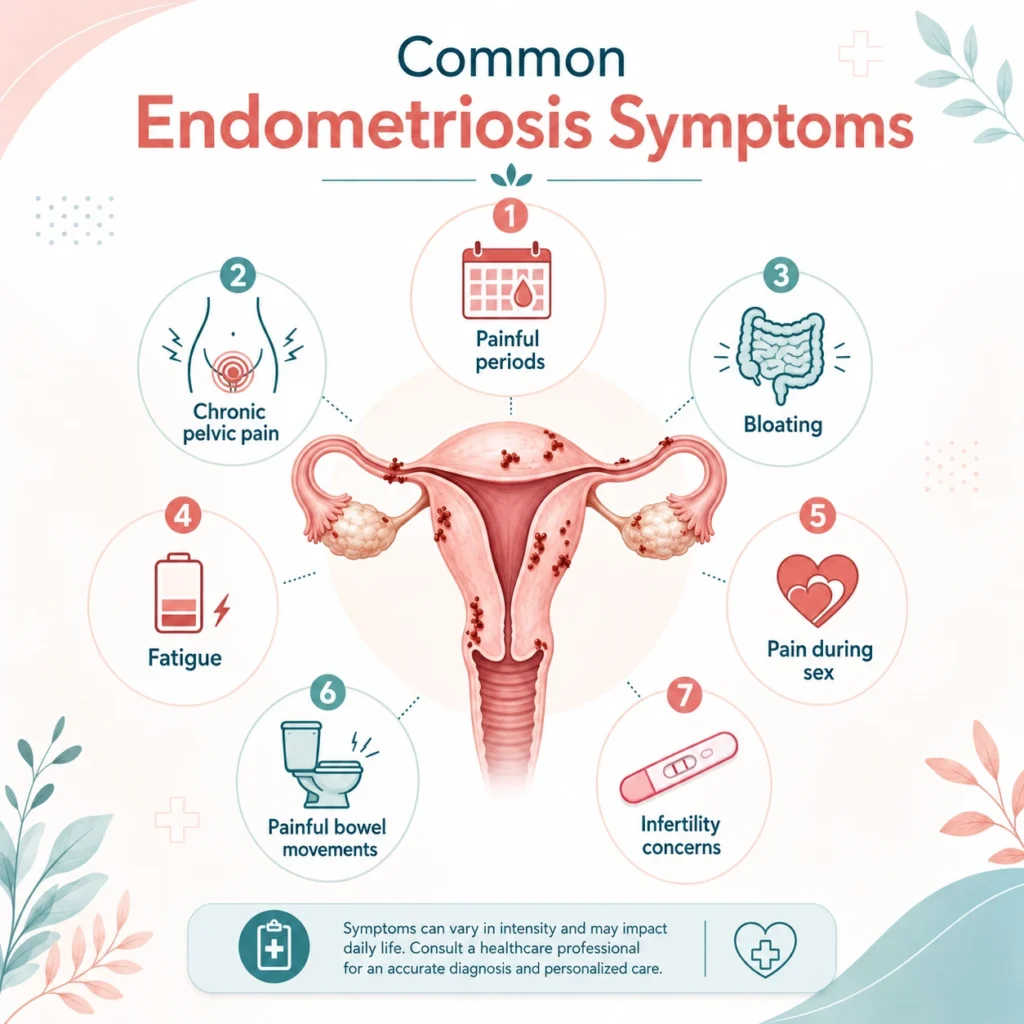
Understanding the full range of endometriosis symptoms is essential because no two women experience this condition in exactly the same way. Some women have severe symptoms with minimal tissue involvement, while others have extensive endometriosis but little pain.
1. Painful Periods (Dysmenorrhoea)
The most recognisable symptom is intense menstrual cramps that worsen over time. Unlike typical period pain signs that improve with over the counter medication, endometriosis related cramps often become debilitating and do not respond to standard pain relief. This pain typically begins one to two days before menstruation and can continue several days into the period.
2. Chronic Pelvic Pain
Pelvic pain in endometriosis is not limited to menstruation. Many women experience a constant, dull ache in the lower abdomen and pelvic region throughout the month. This pain may radiate to the lower back, thighs, or rectum and tends to flare during ovulation or intercourse.
3. Pain During or After Sex (Dyspareunia)
Deep pain during sexual intercourse, particularly with deep penetration, is a classic sign. This occurs when endometrial tissue is present on the uterosacral ligaments or in the cul de sac (the space behind the uterus). Post intercourse pain or spotting may also occur.
4. Heavy Menstrual Bleeding
Women with endometriosis frequently experience heavy or irregular periods, sometimes soaking through a pad or tampon within an hour. They may also have spotting between periods. If you notice significant changes in your menstrual flow, it is worth monitoring alongside other early signs of endometriosis.
5. Painful Bowel Movements or Urination
Endometriosis can affect the bowel and bladder, especially during menstruation. Symptoms include painful bowel movements, diarrhoea, constipation, bloating, and pain when urinating. Rectal bleeding or blood in the urine during a period (though rare) can also indicate endometriosis.
6. Infertility
Endometriosis is found in 20 to 40 per cent of women who struggle with infertility. The condition can affect fertility by distorting the anatomy of the pelvis, causing blockages in the fallopian tubes, impairing egg quality, or creating an environment that is hostile to fertilisation and implantation.
7. Fatigue and Low Energy`
Persistent, unexplained fatigue is common among women with endometriosis. The body is in a constant state of inflammation, which drains energy. This fatigue can be compounded by poor sleep quality due to nighttime pain. If you notice ongoing low energy combined with other symptoms, explore a broader symptoms guide to rule out overlapping conditions.
8. Gastrointestinal Symptoms
Bloating, sometimes called “endo belly”, is one of the most commonly reported but least discussed symptoms. Women may experience such severe bloating that they cannot wear fitted clothing. Nausea, especially around menstruation, is also frequently reported.
9. Shoulder or Chest Pain
In rare cases of diaphragmatic endometriosis, women experience shoulder tip pain or chest discomfort during menstruation. This occurs when endometrial implants are present on the diaphragm and irritate the phrenic nerve.
10. Worsening Symptoms Over Time
One important self check is tracking the progression of symptoms. Unlike conditions that remain stable, endometriosis typically worsens with each menstrual cycle if left untreated. A clear upward trend in pain severity or new symptoms appearing are major red flags.
Still unsure what's causing your symptoms?
How to Self Check for Endometriosis Symptoms
While only a doctor can definitively diagnose endometriosis, there are structured ways to self monitor. Use the following approach
- Keep a symptom diary Track the timing, intensity (on a scale of 1–10), and type of pain you experience throughout the month, not just during your period.
- Note how pain responds to medication. If common NSAIDs like ibuprofen provide little to no relief for menstrual cramps, document this.
- Monitor bowel and bladder changes Record any pain or changes in bathroom habits, particularly around your period.
- Track intercourse related pain Note whether pain occurs before, during, or after sex and its location.
- Photograph your abdomen during bloating episodes Visual documentation can support conversations with your doctor.
Bring this information to your gynaecologist. A thorough history is often the first step toward a diagnosis. Doctors may also recommend a pelvic exam, ultrasound, or MRI to check for cysts, while laparoscopy remains the gold standard for a definitive diagnosis. Keep in mind that thyroid conditions and hormonal imbalances can overlap with endometriosis symptoms, so a comprehensive evaluation is important.
Endometriosis vs. Other Conditions How to Tell the Difference
Because endometriosis shares symptoms with many other conditions, it is easy to confuse. Joint pain and inflammation may point to autoimmune disorders. Chest pain can mimic cardiac issues. Pelvic pain mimics irritable bowel syndrome, interstitial cystitis, pelvic inflammatory disease, and uterine fibroids. The distinguishing factor for endometriosis is the cyclical nature of symptoms tied to the menstrual cycle, combined with a multisystem impact.
If you also experience unexplained weight changes, fatigue, or hair loss, it may be worth asking your doctor to investigate whether endometriosis is occurring alongside another condition such as thyroid disease or an autoimmune disorder.
Treatment Options for Endometriosis
There is currently no cure for endometriosis, but effective management strategies can significantly improve quality of life. Treatment depends on the severity of symptoms, stage of the disease, and whether the woman wishes to conceive.
- Pain management NSAIDs, heat therapy, and, in some cases, low dose opioids for severe flares.
- Hormonal therapy Birth control pills, progestins, GnRH agonists, and hormonal IUDs to suppress the menstrual cycle and slow endometrial growth.
- Surgical intervention Laparoscopy to remove or destroy endometrial implants, cysts, and scar tissue.
- Lifestyle changes Anti inflammatory diet, regular moderate exercise, stress management, and adequate sleep.
- Fertility treatments IUI or IVF, for women struggling to conceive due to endometriosis.
Still unsure what's causing your symptoms?
Frequently Asked Questions
What is the first sign of endometriosis?
The earliest and most common sign is severe period pain that goes beyond typical menstrual cramps and does not improve with standard pain relievers. Many women also notice that their pain has been gradually worsening with each cycle over months or years.
Can you self diagnose endometriosis? N
No, endometriosis cannot be self diagnosed. Only a medical professional can confirm the condition, typically through laparoscopy. However, tracking your symptoms carefully and presenting them to a gynaecologist is a critical first step toward getting a proper diagnosis.
Does endometriosis always cause infertility?
Not always. While endometriosis is a leading cause of infertility, many women with the condition are still able to conceive, either naturally or with medical assistance. The impact on fertility depends on the stage and location of endometriosis.
How is endometriosis pain different from normal period pain?
Normal period pain is typically manageable and lasts one to two days. Endometriosis pain is usually more severe, may begin before the period, continues after it ends, and often doesn’t respond to over the counter pain medication. It may also occur outside of menstruation.
Can endometriosis symptoms appear in teenagers?
Yes. Endometriosis can develop as soon as menstruation begins. Teenagers who experience severe pelvic pain or very heavy periods or are frequently missing school due to period pain should be evaluated by a doctor.
Does endometriosis cause bloating?
Yes. “Endo belly” is a well documented symptom in which the abdomen becomes severely distended, particularly around menstruation. This bloating can be painful and may fluctuate throughout the menstrual cycle, being worse in the days leading up to and during the period.
Is there a blood test for endometriosis?
There is no definitive blood test to diagnose endometriosis. A CA 125 blood test is sometimes used as a supporting tool, but it is not specific to endometriosis and can be elevated in other conditions. Ultrasound and MRI can detect endometriomas, but laparoscopy remains the gold standard for diagnosis.
Can endometriosis go away on its own?
Endometriosis does not typically resolve on its own. However, symptoms may improve temporarily during pregnancy due to hormonal changes, and many women experience significant relief after menopause. Without treatment, the condition tends to persist and may worsen over time.
Can endometriosis affect the bowels and bladder?
Yes. Bowel endometriosis can cause painful bowel movements, bloating, diarrhoea, and constipation, especially around menstruation. Bladder endometriosis can cause painful urination, frequent urination, or blood in the urine during a period.
When should I see a doctor about endometriosis symptoms?
See a doctor if you experience period pain that interferes with daily life, pain during sex, difficulty conceiving, or any of the other symptoms listed in this guide, especially if they are worsening over time. Early consultation is key because delayed diagnosis is linked to more severe disease progression. Keep track of your symptoms and be persistent if your concerns are initially dismissed.